Last Modified: 06/15/2023
Early Hearing Detection and Intervention Quality Improvement Toolkit

Background and Project Overview
The primary aim of the American Academy of Pediatrics (AAP) Early Hearing Detection and Intervention (EHDI) quality improvement project (EHDIQIP) was to make practice-based improvements that lead to enhanced care across the delivery system and strengthen the role of the medical home within the EHDI system by doing the following:
- Increasing the number of newborns who have documentation of the results of their final newborn hearing screening in their medical records by 6 weeks of age;
- Increasing the number of newborns who have documentation in their medical record that the results of the newborn hearing screening were discussed with the family no later than 6 weeks of age;
- Increasing the number of all newborns identified to have risk factors associated with hearing loss, documenting those risk factors in their medical record by 6 weeks of age, and developing individualized care plans by 4 months of age;
- Ensuring children who do not pass their newborn hearing screening have completed an audiological evaluation by 3 months of age and have documentation in their medical record by 4 months of age.
Two phases of the EHDIQIP were implemented over a 13-month period with a total of 11 primary care pediatric practices participating. Six practice teams participated in Phase 1, and five different/new practices teams participated in Phase 2 of this project. Changes were incorporated to the design of Phase 2 based on feedback from Phase 1 participants and lessons learned, including the importance of involving multidisciplinary teams, as well as integrating the participation of a Parent Partner to provide the family perspective as quality improvement measures were implemented and tested. During Phase 2, the pre-work also required an interview of a family with a child who is Deaf or Hard of Hearing to learn more about their experience, identify gaps in the practice related to EHDI processes, and to better able consider the patient/family perspective with each change.
The Quality Improvement Expert Group for Phase 1 consisted of pediatricians and pediatric subspecialists as well as a representative from a nationally recognized family support organization. The Expert Group for Phase 2 expanded to include two additional members who were participants in Phase 1, a primary care pediatrician and an audiologist, who could lend expertise and practical experience to new practice teams.
Project Toolkit
This comprehensive quality improvement toolkit is available as an important resource for AAP EHDI Chapter Champions and other EHDI stakeholders to utilize as they assist pediatricians, AAP chapters, state EHDI programs, clinical practices, and other organizations in implementing a quality improvement and/or Maintenance of Certification project on this topic. All resources are available free of charge and are customizable.
For more information about this project and the resources included below, contact Jamie Jones, Manager, National Resource Center for Patient/Family-Centered Medical Home, American Academy of Pediatrics.
Maintenance of Certification (MOC) and Quality Improvement (QI) Project Materials
Included below is a comprehensive overview that includes information and resources to be used when implementing a QI project focused on EHDI.
Project Planning
Included in this section are resources designed to guide and assist in planning a practice-based quality improvement (QI) project. Sample Institutional Review Board (IRB) and Maintenance of Certification (MOC) Part 4 applications, including supporting documentation, are included.
- Institutional Review Board (IRB) Application [PDF]
- Maintenance of Certification (MOC) Application [PDF]
- Sample Appendices for IRB and MOC Applications
- Recruitment Flier [PDF]
- Recruitment Invitation [PDF]
- Recruitment Application [PDF]
- Practice Team Acceptance Letter [PDF]
- Participant Informed Consent Form [PDF]
- Project Aim Statement and Measures [PDF]
- Chart Record Review Tool – 6 weeks [PDF]
- Chart Record Review Tool – 4 months [PDF]
- Pre- and Post-Implementation Survey [PDF]
- Parent Interview Guide [PDF]
- Parent Partner Engagement Guide [PDF]
- Learning Session Evaluation [PDF]
- Monthly Progress Report [PDF]
- Monthly Educational Webinar Evaluation [PDF]
- Invitation to Participate in Post Project Feedback Call – Parent Partners [PDF]
- Parent Partner Post Project Feedback Call Consent Form [PDF]
- Post-Project Feedback Call – Discussion Guide [PDF]
Pre-work, Orientation and Baseline Data Collection
Important to any Quality Improvement project is the work completed prior to the commencement of data collection. The Pre-Work packet includes a checklist, overview and timeline, activities and instructions for project start-up.
- Pre-Work Packet Materials [PDF]
- Orientation Webinar Presentation
- Pre-Implementation Survey [PDF]
During project pre-work/baseline, records from the prior three months of all infants ages 6 weeks to 4 months who did not pass the newborn hearing screen as well as the records of 20 infants ages 6 weeks and 4 months who did pass the newborn hearing screen per practice (up to 55 medical records total) were reviewed. Record review and data collection of clinical measurements pertinent to the aims of the project were completed using the AAP Quality Improvement Data Aggregator (QIDA).
Members of AAP chapters interested in receiving MOC Part 4 credit for a QI project they are involved with may be eligible to apply for an MOC Part 4 Project through the Academy’s MOC Portfolio Sponsorship. To be eligible, an AAP chapter must have oversight from the national AAP, for example, by using the Quality Improvement Data Aggregator (QIDA) system. For more information about the Academy’s MOC Portfolio Sponsorship, visit the Academy's MOC Portfolio Program page.
Learning Session
An in-person learning session was held at the beginning of the project. Led by Expert Group members, the primary focus was on educating members of the practice teams about quality improvement and EHDI-specific topics. Presentations throughout the EHDIQIP learning session focused on preparing the teams for the activities expected throughout the action periods. Attendees had the opportunity to meet expert group members, as well as participants and parent partners from other practice teams. The opportunity to develop plans in a collaborative environment led to a rich exchange of ideas, solutions, barriers and opportunities.
Materials for the learning session meeting are included below and can be adapted for use.
- Storyboard Template [PDF]
- Learning Session Agenda [PDF]
- Handouts
- Power Point Presentations
- Welcome, Introductions and Project Overview [PDF]
- EHDI: The Role of the Medical Home [PDF]
- Using the Model for Improvement in the Real World/Report on Baseline Data [PDF]
- Parent and Family Perspective – Strategies for Pediatric Practice [PDF]
- State EHDI Programs, Resources from National Technical Assistance Center [PDF]
- Identifying and Managing Risk Factors for Hearing Loss [PDF]
Prior to the in-person Learning Session, the parent partners gathered to get to know one another and share their experiences. This meeting was facilitated by a member of the EHDI QI Expert Group, and allowed parent partners to prepare to be active participants in the learning session alongside their clinical partners.
The Learning Session evaluation provided an opportunity to gain feedback from teams regarding the session itself as well as topics of interest for teams throughout the project.
Action Period
The "action period" is when participants implement small tests of change using project interventions, such as those provided in the change package and learning session. The action period often includes the following activities: monthly data collection via record reviews, completion of brief narrative progress reports, monthly educational webinars, and testing changes using Plan, Do, Study, Act (PDSA) cycles.
Below are resources designed to assist in implementation of all aspects of the action period, including a change package with resources related to Early Hearing Detection and Intervention, sample webinar presentations, listserv and reminder emails, sample Tracking Template, and a Parent Partner Engagement Guide.
- Change Package [PDF]
- Educational Webinars
- ListServ Messages
- Monthly Progress Report [PDF]
- Monthly Educational Webinar Evaluation [PDF]
- Sample Data Collection/Progress Report Reminder Email [PDF]
- Participant Tracking Grid [PDF]
Post Implementation
At the end of the action period, the practice teams completed a post-implementation survey. To compare results, the survey was identical to the pre-implementation survey; it included questions on assessing practice-level care systems for EHDI related topics. The procedure for dissemination and data collection was identical to what was done with the pre-implementation survey.
Resources in this section are designed to assist project organizers in ascertaining successes and challenges outside of the medical record review data, as well as highlight reported practice changes once the action period has concluded. Sample resources include post-implementation surveys, Post-Project Feedback Call Question Guide, MOC Attestation Form, and Certificates of Participation.
- Post- Implementation Survey [PDF]
- Post- Project Feedback Call – Discussion Guide [PDF]
- MOC Attestation Form [PDF]
- Sample MOC Attestation form email [PDF]
- Certificate of Participation [PDF]
Lessons Learned
- Parent partner engagement is an important component of any quality improvement project, but can be challenging due to factors such as time, knowledge of population being served, and access to information. The most effective parent partners were the ones who had lived the experience of having a child who was Deaf or Hard of Hearing, and could share lived experience with the practice team. Engaging a parent takes special consideration of their time and talents.
- Though topics such as risk factors were covered several times throughout the project, there is a need for ongoing education and specific guidance regarding risk factors, assessment, and follow-up. Integration of template reminders within the Electronic Health Record provided ongoing reminders and decision support to practice teams and clinicians to make risk-factor assessment part of ongoing care provision.
- Optimal growth and development for children identified as Deaf or Hard of Hearing is positively impacted when there is timely diagnostic follow-up and referral to early intervention. Because of the changes incorporated, successful identification by 3 months of age, and enrollment into early intervention by 6 months of age was accomplished by practice teams.
- To best meet the needs of both practice staff and patients/families, flexibility is necessary. Teams took the necessary time with families to have conversations about results, and ensure that parents understood the importance of diagnostic testing and enrollment into early intervention.
- For new processes to be fully integrated into practice, it is important that there is multi-disciplinary buy-in throughout the practice for changes to be sustained. Clinicians, office staff, and parent partners were all part of ensuring that changes occurred systematically.
- Integration of templates and reminders within Electronic Health Record (EHR) systems made a key difference to the consistency in which conversations, assessments, and follow-up occurred. By having these reminders, care providers could address the issues related to early hearing detection and intervention.
Results
Project participants were asked to submit baseline data from the prior three months of all infants ages 6 weeks to 4 months who did not pass the newborn hearing screen as well as the records of 20 infants ages 6 weeks and 4 months who did pass the newborn hearing screen per practice—up to 55 medical records total. Record review and data collection of clinical measurements pertinent to the aims of the project were completed using the AAP Quality Improvement Data Aggregator (QIDA).
For the following six subsequent months, participants were asked to submit 20 patient record reviews using a web-based data aggregation tool (QIDA), for a total of 7 cycles of data collection.
Measures and outcomes for this project are as follows:
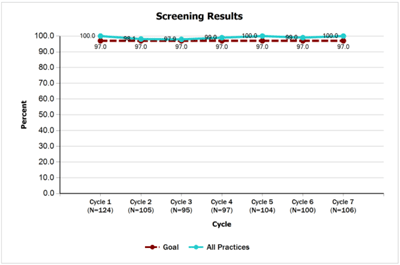
- 97% or more of all newborns have documentation of the results of their final newborn hearing screening in their medical records by 6 weeks of age. Teams consistently performed well on this measure throughout the project with all teams performing at or above the measure goal.
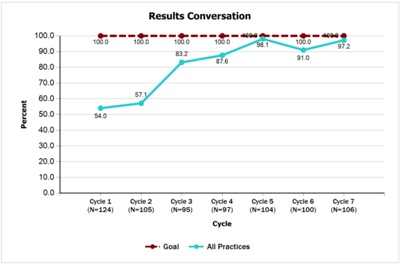
- 97% of newborns have documentation in their medical record that the results of the newborn hearing screening were discussed with the family no later than 6 weeks of age. Teams made significant improvements on this measure with 54% discussing the results with families at baseline versus 97.2% at the end of the project.
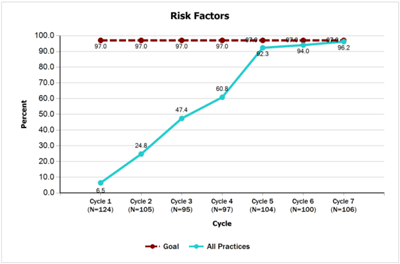
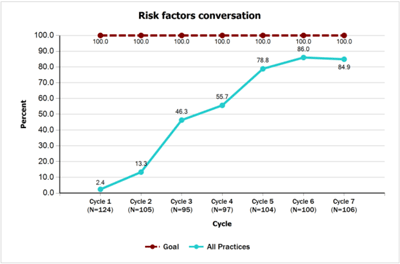
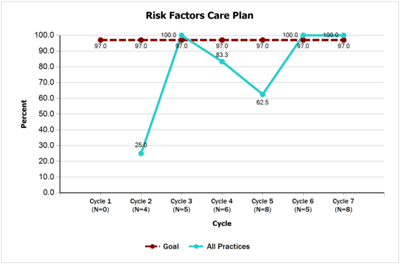
- 97% or more of all newborns identified to have risk factors associated with hearing loss will have documentation of those risk factors in their medical record by 6 weeks of age and will have an individualized care plan by the 4 months of age. Teams made significant improvements on this measure with 6.5% documenting risk factors at baseline versus 96.2% by the end of the project. Teams also made significant improvement on developing individualized care plans for at-risk patients—moving from 25% at baseline to 100% by the end of the project.
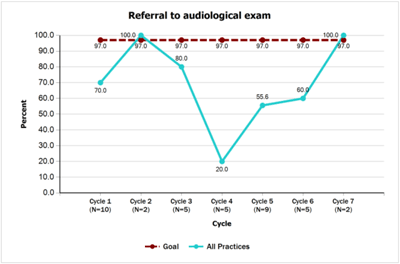
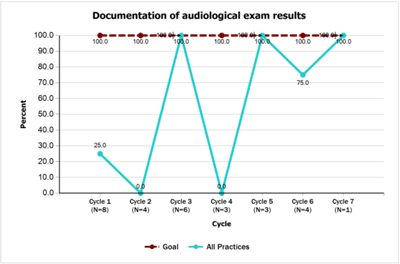
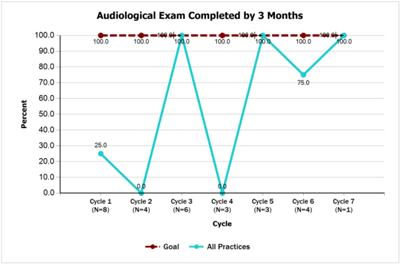
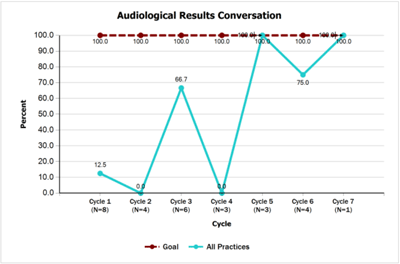
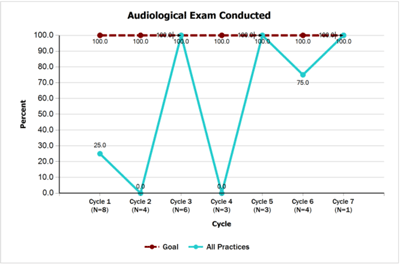
- 100% of children who do not pass their newborn hearing screening have completed an audiological evaluation by 3 months of age and documentation will be in their medical record by 4 months of age. Teams accomplished the goal on this measure and by the end of the project had achieved 100% for both audiological evaluation and documentation of results as compared to 25% at baseline.
- Final Report [PDF]
- Executive Summary [PDF]
Final Chart Runs:
Project Aggregate – 6-Weeks Tool – Final Data
All Measures (Record Review Tool-6 Weeks [Practice])
All Practices Report for All Participants/Practices : 8/1/2017
6-Weeks Tool:
- Screening Results [PDF]
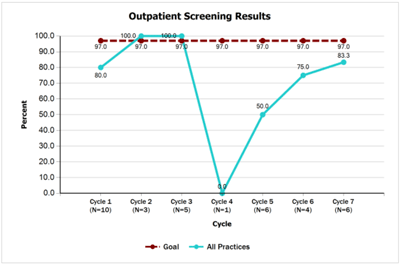
- Outpatient Screening Results [PDF]
- Referral to Audiological Exam [PDF]
- Results Conversation [PDF]
- Risk Factors [PDF]
- Risk Factors Conversation [PDF]
Project Aggregate – 4-Month Tool - Final Data
All Measures (Record Review Tool-4 Months [Practice])
All Practices Report for All Participants/Practices : 8/1/2017
4-Month Tool:
- Audiological Exam Conducted [PDF]
- Audiological Exam Completed by 3 Months [PDF]
- Documentation of Audiological Exam Results [PDF]
- Audiological Results Conversation [PDF]
- Risk Factor Care Plan [PDF]
Additional project highlights include the following:
- Significant improvements were made in results documentation, conversations with families, risk factor assessment and referrals for diagnostic testing.
- There was a marked increase in awareness and usage of Early Hearing Detection and Intervention (EHDI) Guidelines for Pediatric Medical Home Providers [PDF].
- During the last 3 data cycles, 100% of participants reported that though additional assessments around risk-factors were being done, physicians could maintain their schedules, and office wait times remained the same.
Acknowledgement of Support, Contact Information for Additional Information
This project was supported by a cooperative agreement funded by the Maternal and Child Health Bureau (MCHB). Its contents are solely the responsibility of the site content authors and do not necessarily represent the official views of the MCHB or the United States Department of Health and Human Services.
For more information about Early Hearing Detection and Intervention tools, resources and materials, visit aap.org/EHDI, or contact Sandi Ring, Program Manager, Early Hearing Detection and Intervention, Division of Children with Special Needs, American Academy of Pediatrics.
For more information about Quality Improvement (QI) at the AAP, including how to participate in QI initiatives, view the quality improvement section of the AAP website. Visit the AAP Website for additional information about its Maintenance of Certification Portfolio Program.


